“The beauty of a woman is not in the clothes she wears, but in the confidence she owns.” – Audrey Hepburn’s words remind us that self-assurance starts with feeling comfortable in our own bodies. When discomfort stems from a visible issue, like persistent roughness or flaking, it demands both compassion and science-backed solutions.
This Website contains affiliate links. That means I may earn a small commission if you purchase through my links, at no extra cost to you.
Xeroderma, the medical term for this common issue, occurs when the epidermis loses moisture and sheds in large flakes. Many confuse it with temporary dryness, but true scaling involves deeper layers and often signals an imbalance. Through years of research and firsthand experience, I’ve learned that proper identification separates temporary fixes from lasting results.
This guide breaks down the biology behind flaking and how it differs from similar conditions. You’ll discover why generic lotions fail and how tailored strategies address root causes. My approach merges dermatological insights with actionable steps—no guesswork required.
Key Takeaways
- Learn the medical science behind moisture loss and flaking (xeroderma).
- Discover how to distinguish between basic dryness and chronic scaling.
- Explore evidence-based methods to restore your epidermis’s natural balance.
- Understand why personalized care outperforms one-size-fits-all products.
- Gain tools to improve both comfort and confidence long-term.
Introduction to My Journey with Dry Scaly Skin
Like countless others, I woke up one morning to find my confidence crumbling under patches I couldn’t ignore. What began as minor irritation escalated into relentless flaking that mocked every cream I tried. This wasn’t just about appearance—it felt like my body had declared war on itself.
My Personal Experience and Initial Struggles
I spent months cycling through drugstore aisles, hoping the next lotion would be the solution. Nothing stopped the tightness or peeling. The more I treated it like basic dryness, the worse the symptoms became. Friends suggested home remedies, but coconut oil and oatmeal masks only provided fleeting relief.
Three critical realizations changed everything:
- Visible texture changes often signal deeper skin imbalances
- Overwashing exacerbated my condition
- Generic products lack targeted ingredients for severe cases
Why This Guide Means So Much to Me
Through healthcare consultations, I learned my struggle wasn’t unique. Many people hide their discomfort, fearing judgment about flakes or redness. This guide distills every lesson from:
- Clinical research on epidermal repair
- Dermatologist-recommended protocols
- Personal trials with prescription-grade solutions
Understanding the severity spectrum transformed my approach. What calms mild irritation won’t address cracked patches. Now, I want others to skip the guesswork and reclaim their comfort—one informed choice at a time.
Understanding Dry Scaly Skin: Causes and Symptoms
When I first noticed rough patches on my elbows, I brushed it off as temporary irritation. Little did I know, these changes signaled deeper cellular disruptions requiring more than basic moisturizers. Identifying the root cause became my turning point.
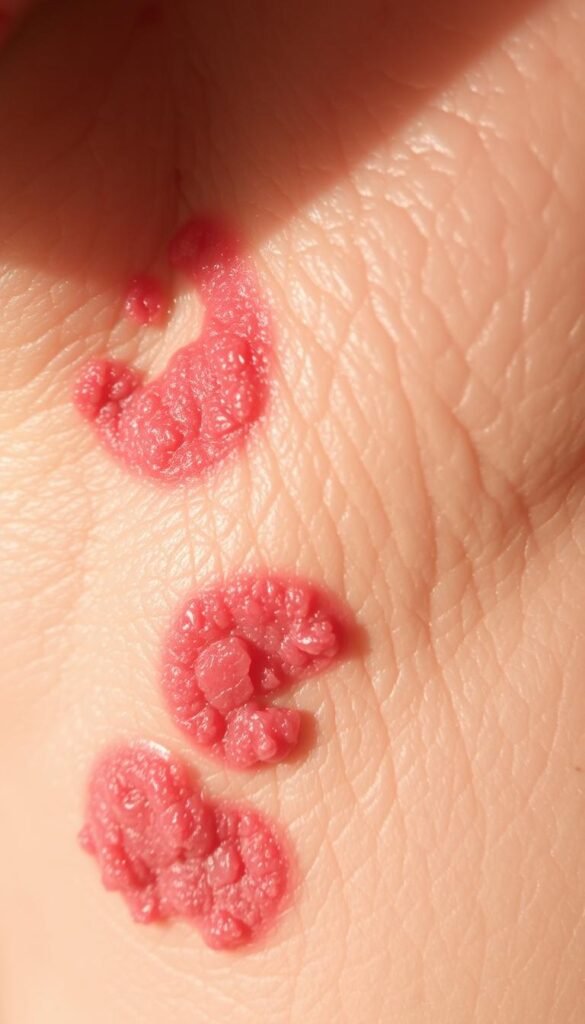
Common Causes and Triggers
Through trial and error, I discovered multiple culprits behind persistent flaking. Environmental factors like arid climates strip natural oils, while harsh chemicals in cleaning products damage protective barriers. One dermatologist explained, “Contact dermatitis often mimics dryness but involves immune responses to irritants like nickel or formaldehyde.”
Recognizing the Symptoms and Warning Signs
Itching and redness initially confused me. Over time, I learned to differentiate between temporary discomfort and chronic issues. Psoriasis creates silvery scales, while eczema produces weepy patches. Watch for these indicators:
| Condition | Texture | Pattern |
|---|---|---|
| Allergic Reaction | Bumpy | Irregular borders |
| Eczema | Leathery | Flexure areas |
| Psoriasis | Thick plaques | Symmetrical |
Insights from Healthcare Experts
Dr. Alicia Torres, a board-certified dermatologist, stresses: “Persistent scaling with swelling or pus warrants immediate evaluation—it could signal infections or autoimmune activity.” Tracking symptom duration and spread helps professionals distinguish between dermatitis types and prescribe targeted solutions.
My Step-by-Step At-Home Treatment Approach
After years of trial and error, I developed a battle-tested system that combines science-backed products with gentle care. This method transformed my toughest texture issues into smooth, resilient surfaces—without expensive procedures.

Effective Over-the-Counter Remedies I Use
Three ingredients became game-changers in my routine. Creams with urea or lactic acid gently exfoliate while locking in moisture. For stubborn patches, I layer petroleum-based ointments as overnight masks. My dermatologist-approved process:
- Cleanse with pH-balanced formulas
- Apply treatment creams to affected areas
- Seal with occlusive balms
| Product Type | Key Ingredients | Best For |
|---|---|---|
| Exfoliating Cream | Urea 10%, Ceramides | Rough elbows/knees |
| Moisturizing Ointment | Petrolatum, Dimethicone | Cracked fingertips |
| Soothing Lotion | Colloidal Oatmeal, Glycerin | Itchy dermatitis areas |
Natural Home Remedies That Have Worked for Me
While clinical treatments form my foundation, these additions accelerate healing. Cool oatmeal baths calm irritation within minutes. I mix raw honey with aloe vera gel for spot treatments—nature’s antibacterial duo. Three rules I follow:
- Apply natural remedies to clean, dry skin
- Test small parts before full application
- Combine with prescribed treatments when needed
Consistency matters more than any single product. I treat all affected areas daily, even when improvements appear. This prevents recurring flare-ups and maintains my progress.
Professional and Prescription Treatment Options
Breaking free from stubborn texture issues sometimes requires more than DIY solutions. During my third dermatology visit, I realized persistent problems demand professional insight. “Self-treatment has limits,” my doctor noted. Specialized care became my turning point.
When to Seek Medical Advice
I learned to watch for red flags after weeks of failed OTC attempts. Swollen areas or yellow crusting signaled possible infections. My rule: If itching disrupts sleep or spreads rapidly, schedule an appointment. Fever with widespread irritation? That’s ER territory.
Prescription Creams and Advanced Therapies
Dermatologists prescribed targeted solutions I’d never considered. A cortisone cream halted my worst flare-up in days. For chronic cases, options expand:
| Treatment Type | Active Ingredients | Best For |
|---|---|---|
| Topical Immunomodulators | Tacrolimus, Pimecrolimus | Face/neck sensitivity |
| Phototherapy | UVB Light | Psoriasis patches |
| Biologic Injections | Dupilumab | Severe eczema |
One surprising lesson: Untreated scaling invites complications. Bacterial infections required antibiotics during my journey. Now, I prioritize early intervention through trusted healthcare services.
Daily Care Routines and Lifestyle Modifications
Consistency transformed my approach to managing persistent texture issues. What began as tedious maintenance evolved into effortless habits that keep my body balanced year-round. Let me walk you through strategies that work with real-life demands.
Creating a Skincare Routine That Fits My Life
Mornings start with a featherlight moisturizer for my face and richer creams for high-friction areas like elbows. At night, I switch to barrier-repair formulas that combat moisture loss while I sleep. Three non-negotiables:
- Gentle sulfate-free cleansers for my scalp and body
- Broad-spectrum sunscreen reapplied every two hours in sun
- Targeted treatments for active flare-ups
Lifestyle Changes That Help Prevent Flare-Ups
I discovered environmental tweaks matter as much as topical care. A bedroom humidifier prevents winter-induced cracking on my legs. Stress management techniques like breathwork reduced facial irritation linked to my condition. Key adjustments:
- Swapped harsh detergents for fragrance-free alternatives
- Identified fabric triggers (wool = instant itch)
- Prioritized hydration tracking via water intake apps
These shifts didn’t happen overnight. I implemented one change weekly until they became second nature. Now, my skin stays resilient through travel, stress, and seasonal shifts.
Addressing Underlying Conditions and Complications
Navigating persistent texture issues taught me that surface treatments only scratch the problem’s depth. Many visible changes stem from conditions requiring specialized approaches. From seborrheic dermatitis’s oily crusts to psoriasis’s thick plaques, recognizing these patterns transformed my care strategy.
Managing Allergic Reactions and Infections
I once mistook an allergic reaction for routine irritation until swelling spread across my arms. Now, I act immediately when rashes appear suddenly. “Delayed treatment invites secondary infections,” warns Dr. Elena Martinez, my allergist. Three lessons guide my protocol:
- Track exposure to new products or foods
- Use antihistamines for sudden flare-ups
- Apply prescribed antibiotic creams to broken areas
| Complication | Signs | Action Steps |
|---|---|---|
| Bacterial Infection | Yellow crusting, warmth | Oral antibiotics |
| Fungal Overgrowth | Circular red patches | Antifungal shampoos |
| Contact Dermatitis | Linear rash pattern | Steroid creams |
Dealing with Related Skin Conditions
My scalp’s stubborn flakes revealed seborrheic dermatitis—a condition thriving in oily zones. Unlike standard moisturizers, ketoconazole shampoos became my salvation. For eczema on my elbows, I combine:
- Colloidal oatmeal baths
- Calcineurin inhibitors
- Strict allergen avoidance
Psoriasis demanded a different tactic. Phototherapy sessions reduced plaque thickness better than any cream. Through trial and error, I learned each condition’s unique rules:
| Condition | Key Feature | Management |
|---|---|---|
| Eczema | Weeping patches | Barrier repair creams |
| Psoriasis | Silvery scales | UV light therapy |
| Seborrheic Dermatitis | Oily crusts | Antifungal agents |
Conclusion
Through years of trial and insight, I’ve learned that managing texture changes requires both knowledge and self-compassion. While these visible concerns might feel isolating, effective solutions exist when you address root causes—whether environmental triggers, seborrheic conditions, or immune responses.
Consulting healthcare professionals transformed my approach. They helped me distinguish between temporary irritation and chronic issues needing targeted treatment. For example, persistent rashes on sun-exposed areas often signal deeper imbalances, while eczema requires different care than psoriasis.
Proactive prevention matters most. I now prioritize gentle products for sensitive body parts and monitor for early signs of complications. Simple habits—like tracking moisture levels and minimizing allergen exposure—maintain my progress better than any quick fix.
Remember: Your comfort matters. With the right strategies, even stubborn patches become manageable. Let this guide empower you to seek solutions that restore both your skin’s health and your confidence.





